During a comprehensive eye exam, our optometrists do more than just determine your prescription for eyeglasses. We further assess how your eyes work together as a team, exam your eyes for any ocular conditions or diseases, and evaluate your eyes as an indicator of your overall health.
It is recommended you have an eye exam yearly to monitor your ocular health and visual function. The eye exam can take 30 minutes to 1 hour, depending on your visual needs.
Below are a series of tests you are likely to encounter during a comprehensive eye exam. Each test evaluates a different aspect of your vision.
Visual Acuity Test
Visual acuity measurements evaluate how clearly you can see. The tests usually involve reading letters or looking at symbols of different sizes on an eye chart at near and far distances. Each eye is tested individually. Then both eyes may be tested together, with and without corrective lenses (if you wear them).
Preliminary Tests: Color Vision, Stereoposis, Autorefraction / Autokeratometry
Preliminary tests such as color vision, stereoposis, and autorefraction and autokeratometry may be performed to evaluate specific aspects of your visual function and eye health.
- Color Vision Test: Color vision tests assess your ability to distinguish colors. It is used to screen for hereditary color vision deficiency or color blindness in people with suspected eye diseases.
- Stereoposis Test: Stereopsis testing measures depth perception, the process by which we perceive the world in three dimensions.
- Autorefraction/Autokeratometry: Your optometrist may use an autorefractor/autokeratometer to obtain an approximation of your prescription and curvature of your cornea. During autorefraction, you look at a picture in a computer- controlled machine. The picture moves in and out of focus as the machine takes readings to determine when the image is on the retina. Several readings are taken and averaged to form a prescription. No feedback is required from you during this process.
Pupils
Pupil testing, a neurological procedure performed by your optometrist, assesses the automatic reflex of your pupils in response to light. A light will be shine into your eyes from each side and swing rhythmically from one eye to another. Your optometrist will watch your pupils closely to determine whether or not your pupils constrict in response to the light, making note of the size and shape of your pupils.
Eye Focusing, Eye Teaming, and Eye Movement Testing
Assessment of accommodation, ocular motility and binocular vision determines how well the eyes focus, move and work together. In order to obtain a clear, single image of what is being viewed, the eyes must effectively change focus, move and work in unison. This testing will look for problems that keep your eyes from focusing effectively or make using both eyes together difficult.
 Retinoscopy
Retinoscopy
Your optometrist may perform retinoscopy to obtain an approximate measurement of your prescription. During retinoscopy, the exam room lights will be dimmed and you will be given a large target (usually the big “E” on the chart) to fixate on. As you stare at the “E,” your optometrist will shine a light at your eye and flip lenses in a machine in front of your eyes.
Refraction
During a refraction assessment, your optometrist puts a mask-like instrument called a phoropter in front of your eyes and shows you a series of lens choices. He or she will then ask you which of the two lenses in each choice looks clearer. Based on your responses, your optometrist will determine your exact eyeglass prescription to give you the sharpest vision. Refraction determines whether you have hyperopia (farsightedness), myopia (nearsightedness), astigmatism, and/or presbyopia.

Slit-Lamp Examination
The slit lamp exam uses an instrument similar to a microscope to provide a magnified, three-dimensional (3-D) view of the different parts of the eye. The microscope focuses an intense narrow line of light on your eye. This procedure allows your optometrist to thoroughly evaluate your eye health and detect any signs of infection or disease, including conjunctivitis, cataracts, macular degeneration, diabetic retinopathy, and retinal detachment.
Tonometry: The Glaucoma Test
Tonometry measures the intraocular pressure of the eyes. There are several different versions.
The most common glaucoma test is the “puff-of-air” test, technically known as non-contact tonometry, or NCT. During NCT, a small burst of air is puffed at your open eye. It is completely painless, and the tonometer does not touch your eye.
Another type of glaucoma test is performed with a probe called an applanation tonometer that is mounted on a slit-lamp. During applanation tonometry, eye drops are used to numb the eye. Then your optometrist will have you stare straight ahead as he or she gently touches the surface of your eye with the tonometer to measure your intraocular pressure. This is a painless and quick procedure.
Pupil Dilation
In order to better assess the back of your eye, your optometrist may instill dilating eye drops to enlarge your pupils. Dilating eye drops usually take about 20 to 30 minutes to take effect. When your pupils are dilated, you will be sensitive to light and you may notice difficulty focusing at near. These effects can last from 4 to 6 hours, depending on the strength of the dilating drops used. Once the drops have taken effect, your optometrist will use various high intensified instruments to assess the internal structures of your eyes.
Visual Field Test
A visual field test measures how much peripheral or “side” vision you have. During automated perimetry, a computer-controlled machine such as the Humphrey Field Analyzer is used. You sit in front of a concave dome focusing on a target in the center. Random lights of different intensities are flashed in your peripheral field of vision. You click the button whenever a light is seen. The computer then automatically maps and calculates your visual field. Visual field tests can detect central and peripheral vision problems caused by glaucoma, stroke and other eye or brain problems.
Specialized Tests
As part of your comprehensive eye examination, we recommend additional specialized procedures called retinal photography and optical coherence tomography.
Retinal Photography: Retinal imaging is a technique consisting of capturing an image of the retina (back of the eye). This is not an X-ray or ultrasound procedure. High-resolution digital photographs of the retina are simply and safely taken. This permanent record is invaluable in assessing the current health of your eye; and for safeguarding the health of specific structures of your retina. It will also serve as a baseline for comparison with previous and subsequent visits.
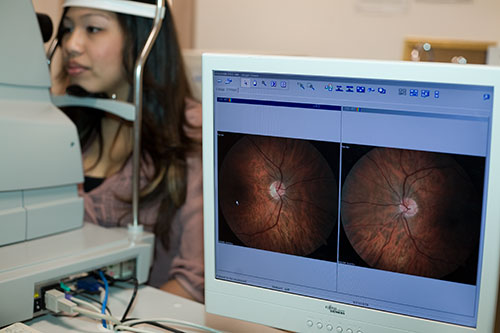
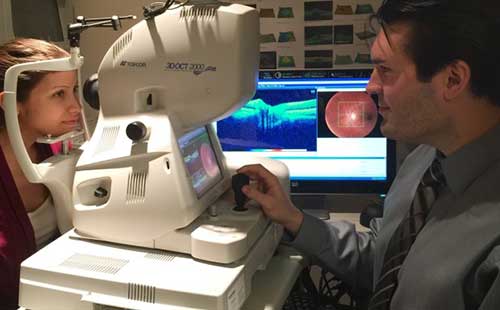
Optical Coherence Tomography (OCT): OCT is a non-invasive technology used for imaging the retina, the multi-layered sensory tissue lining the back of the eye. OCT, the first instrument to allow doctors to see cross-sectional images of the retina, is revolutionizing the early detection and treatment of eye conditions such as macular holes, pre-retinal membranes, macular swelling and even optic nerve damage.
Completion of Examination
At the completion of the examination, your optometrist will assess and evaluate the results of all the tests to determine a diagnosis and develop a treatment plan. He or she will discuss with you the nature of any visual or eye health problems found and explain available management options. In some cases, referral for consultation with or treatment by another eye care or health care provider may be indicated.



Add comment